New research from Washington State University just revealed something paradoxical about chronic insomnia. When researchers subjected both healthy sleepers and people with insomnia to 38 hours of total sleep deprivation, the insomnia group showed preserved decision-making ability before a rule change but completely fell apart afterward.
The secret? Hyperarousal.
People with chronic insomnia exist in a constant state of excessive brain activation. This hyperarousal actually protected their performance during straightforward tasks but destroyed their ability to adapt when circumstances changed. The same neural state that keeps them functioning through exhaustion also locks their brain into rigid patterns that can’t shift when flexibility matters most.
And every study on this topic keeps missing the fundamental point. The gloss over what describes hyperarousal. Researchers measure its effects. But they seldom state what hyperarousal actually is at its source.
It’s not some vague state of “being alert.” Hyperarousal has a distinct neurological signature that is evident on EEG recordings. High-frequency beta brainwave activity, running at 15-35 hertz, floods the prefrontal cortex. Your brain’s executive control center runs in overdrive 24 hours a day, processing information at frequencies that should only appear during intense focus or stress.
What Hyperarousal Actually Looks Like
When researchers measure brain activity in people with chronic insomnia, they find elevated beta waves throughout the day and night. This high-frequency activity persists during sleep onset, continues through non-REM sleep, and remains elevated even during the deepest stages of sleep.
Studies using high-density EEG reveal that this pattern centers specifically in the prefrontal cortex. While insomnia patients show elevated beta activity across multiple brain regions, the prefrontal areas demonstrate a unique signature. During sleep, healthy brains show decreased beta and increased delta waves in the prefrontal cortex. Insomnia brains show beta activity that resembles waking consciousness more than sleep.
The prefrontal cortex functions as a Grand Central Station for learning and memory. This region coordinates executive functions, including working memory, decision-making, planning, and cognitive flexibility. Prefrontal networks process every new piece of information you learn. Every decision you make engages these neural circuits. Every time you need to shift strategies or adapt to changing circumstances, your prefrontal cortex orchestrates that transition.
Now imagine running Grand Central Station at rush-hour intensity 24/7. No breaks. No quiet periods. Constant high-speed processing that never stops.
That’s what hyperarousal creates in the brains of people with chronic insomnia.
The Frequency and Amplitude Problem
Here’s what research studies consistently fail to emphasize. Hyperarousal doesn’t exist as some abstract concept. It manifests as measurable changes in brainwave frequency and amplitude that appear on every EEG recording.
Beta wave activity between 15 and 35 hertz increases significantly in insomnia patients compared to healthy sleepers. This anomaly happens during wakefulness, during attempted sleep, and throughout all sleep stages. The amplitude of these high-frequency waves stays elevated while the amplitude of slow-wave delta activity decreases.
People with chronic insomnia show beta dominance when their brains should produce delta and theta—the frequency distribution shifts toward fast activity that prevents deep restorative sleep. The amplitude measurements show excessive power in frequencies associated with arousal and insufficient power in frequencies associated with sleep.
Research tracking insomnia patients during the middle of the day confirms that this pattern persists around the clock. At 2 PM, when most people feel alert and focused, insomnia patients show beta activity levels that exceed those of healthy brains. Their baseline arousal state already maxes out the frequencies that should only spike during demanding cognitive tasks.
Why This Wrecks Executive Function
The Washington State study demonstrates the cognitive cost. Researchers used a reversal-learning task in which participants learned a rule, applied it successfully, and then had to adapt when the rule changed without warning.
Before the reversal, insomnia patients under sleep deprivation performed remarkably well. Their hyperarousal compensated for the lack of sleep. The excessive beta activity in their prefrontal cortex kept them alert and functional for straightforward decision-making.
Then the rule changed.
Suddenly, the strategies that worked stopped working. Participants needed to recognize the shift, abandon their established approach, and develop a new strategy. This task requires cognitive flexibility, the ability to shift mental sets and adapt to changing circumstances.
The insomnia group collapsed. Their performance dropped significantly more than that of healthy sleepers attempting the same task.
Hyperarousal creates cognitive rigidity. The constant high-frequency activation locks your prefrontal cortex into existing patterns. You can execute established routines effectively. You maintain focus on familiar tasks. But when circumstances demand flexibility, when you need to shift gears or see problems from a new angle, that locked-in activation pattern becomes a cage.
The Prefrontal Cortex Under Siege
Multiple brain imaging studies show that chronic hyperarousal disrupts the normal functioning of prefrontal networks. This region typically coordinates multiple cognitive processes through dynamic shifts in activation patterns. Different tasks engage different prefrontal sub-regions in different combinations.
But constant beta dominance interferes with this dynamic coordination. The prefrontal cortex can’t smoothly shift between processing modes when it’s stuck in a perpetual state of high-frequency activation.
Think about learning new information. Your brain needs to encode incoming data, compare it to existing knowledge, create new associations, and consolidate those connections into long-term memory. This process requires coordinated activity across multiple frequency bands.
Research on adolescents with insomnia reveals this pattern emerges early. Even young people with insomnia show elevated beta activity during sleep attempts and throughout sleep stages. The hyperarousal signature appears before other psychiatric disorders develop, suggesting it functions as a core feature rather than a consequence.
The 24-Hour Problem
Most people assume insomnia only affects nighttime. You can’t sleep, but once morning arrives, you function normally during the day.
Wrong.
EEG studies measuring daytime brain activity demonstrate that hyperarousal persists throughout waking hours. The elevated beta frequency, the excessive amplitude in high-frequency bands, and the reduced slow-wave activity in frontal regions persist from morning through the afternoon into the evening.
Sadly, it creates cumulative damage—every hour of hyperarousal taxes your prefrontal networks. Every day without proper slow-wave sleep prevents the restoration your brain desperately needs. Every week of continuous beta dominance further entrenches the pattern.
Studies using transcranial direct current stimulation aimed to reduce cortical excitability in the prefrontal cortex of patients with insomnia. The intervention worked for healthy controls but failed for people with chronic insomnia. Their baseline hyperarousal proved so persistent that even direct electrical manipulation couldn’t override it.
The researchers concluded that persistent hyperarousal fundamentally alters how the brain responds to interventions. Treatments that work for healthy brains encounter different neural terrain in chronically hyperaroused systems.
Learning and Memory Take the Hit
Memory formation requires orchestrated activity across multiple brain regions and frequency bands. The prefrontal cortex coordinates this process but can’t execute it effectively under constant hyperarousal.
Research on working memory in patients with insomnia shows preserved basic functions but impaired flexibility. You can hold information in mind and manipulate it according to familiar rules. But introduce novel demands or require strategic shifts, and performance degrades rapidly.
It also explains a common experience among people with chronic insomnia. You feel mentally sharp for routine tasks. You can focus intensely on familiar work. But learning genuinely new material becomes exhausting. Solving problems that require creative approaches feels nearly impossible. Adapting to unexpected changes overwhelms your cognitive capacity.
Your prefrontal cortex stays active but loses its flexibility. The hyperarousal that keeps you functioning simultaneously also prevents the neural dynamics required for complex learning and adaptive thinking.
Where Studies Go Wrong
Almost every research paper on insomnia and hyperarousal describes the phenomenon, measures its correlates, and documents its effects. Very few emphasize the fundamental neurological signature.
Hyperarousal is characterized by excessive beta-frequency EEG activity with elevated amplitude, centered in prefrontal cortex regions.
That’s not a vague state. It’s a measurable, quantifiable pattern that consistently appears across studies, populations, and measurement techniques. You can see it on every EEG recording. You can track it across the 24-hour cycle. You can measure its intensity and monitor how it changes over time.
Studies measure heart rate variability, cortisol levels, metabolic activity, and cognitive performance—all of these correlate with hyperarousal. But the core issue appears in brainwave frequency and amplitude measurements.
Fix the EEG pattern, and the secondary markers improve. Reduce beta dominance, restore delta wave production during sleep, reestablish normal frequency distributions across the 24-hour cycle, and cognitive function recovers.
Treat the secondary markers while leaving the brainwave pattern unchanged, and improvements remain limited or temporary.
How Sleep Recovery Addresses Hyperarousal
At Sleep Recovery, we’ve worked with hyperarousal for 17 years through alpha-theta neurofeedback. The approach targets the exact brainwave patterns that maintain chronic insomnia.
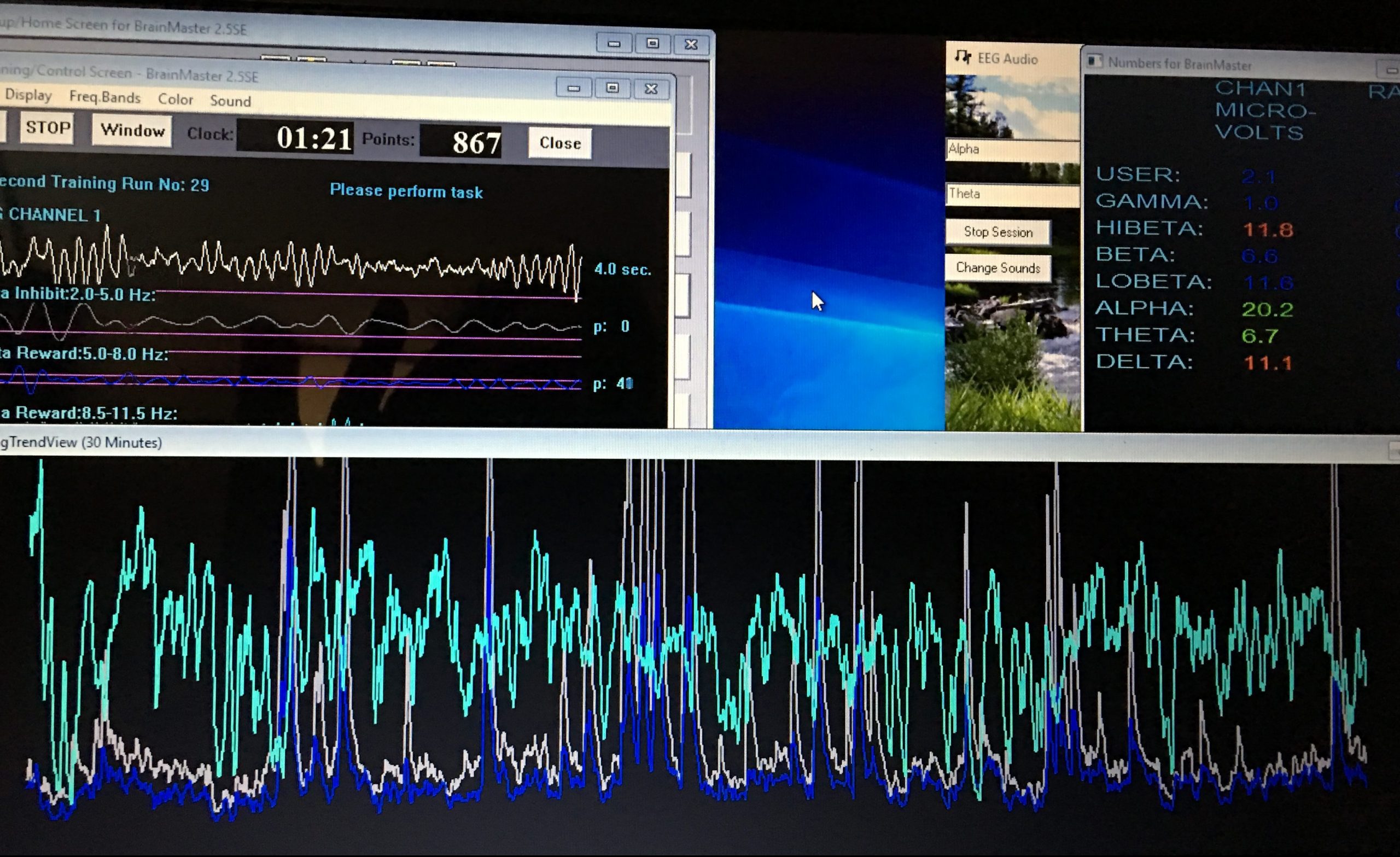
We monitor beta frequency and amplitude in prefrontal regions alongside alpha and theta production. The neurofeedback system provides immediate visual and auditory feedback showing when beta activity decreases and when alpha-theta patterns emerge.
Most people with chronic insomnia have never experienced what normal prefrontal activity feels like. They’ve run at maximum beta frequency for so long that hyperarousal seems like their natural state. The neurofeedback training teaches their nervous system what reduced arousal actually means.
Sessions typically last 30 minutes. Clients’ brains practice shifting out of beta dominance into alpha-theta ranges, where the brain can actually rest. The training doesn’t rely on conscious effort or cognitive strategies. You can’t think your way out of hyperarousal because thinking engages the exact prefrontal networks that need to quiet down.
Instead, the neurofeedback provides direct information about your current brainwave state. When beta amplitude decreases, you get positive auditory feedback. When alpha or theta waves increase, you receive alternative sounds of reinforcement. Your nervous system learns through repeated exposure to these states.
The pattern starts changing within 10-12 sessions for most clients. Beta dominance begins loosening. Prefrontal regions begin to produce normal frequency distributions. Clients report feeling something they haven’t experienced in years: actual mental rest.
As the EEG pattern normalizes, executive function improves. Working memory becomes more flexible. Learning new information requires less effort. Adapting to changing circumstances no longer overwhelms cognitive capacity. The Grand Central Station of your brain finally gets periods of reduced traffic instead of running at rush hour intensity 24/7.
More importantly, sleep quality improves as beta activity decreases during nighttime hours. Delta waves start appearing during deep sleep stages. The brain begins cycling through normal frequency patterns instead of maintaining constant high-frequency activation.
The Path Forward
Hyperarousal doesn’t happen because people with insomnia choose to stay alert. It’s not a matter of relaxation techniques or sleep hygiene. The brainwave pattern develops through complex interactions between stress systems, sleep-wake regulation, and neural plasticity.
But once established, it maintains itself in the long term through the same neural mechanisms. Human brains are not three pounds of stupid. They are highly and autonomously self-intelligent. And once it learns new, more efficient ways of managing its own EEG flow, it forgets it or unlearns it.
Your prefrontal cortex doesn’t need to run at maximum frequency 24 hours a day. Grand Central Station can have quiet periods. Learning and memory can function through coordinated frequency patterns instead of constant high-frequency activation.
After 17 years of working with thousands of clients, the pattern holds consistently. Address the brainwave signature, and everything else follows. Ignore the EEG fundamentals, and improvements remain superficial no matter what other interventions you try.
Hyperarousal isn’t mysterious. It’s measurable, trackable, and most importantly, changeable. The question is whether you’ll address it at its actual source or keep treating secondary symptoms while the core pattern persists.
For more info on this approach, visit: https://sleeprecovery.net or call: 800 927 2339