Financial Problems of the Elderly: America’s New Affordability Shock

Seniors and the elderly in the US and the EU are facing serious difficulties both financially and neurologically.
Edith H. is one of those affected. It started when her husband’s pension got cut—not eliminated — cut. Enough to matter, not enough to qualify for any assistance. She runs the numbers every night before bed, sometimes literally with a calculator on the nightstand. Groceries, utilities, and the co-pay she keeps putting off. By the time she’s done, sleep is gone. And in the morning, she can’t remember where she put her keys, whether she took her blood pressure medication, or what her daughter said on the phone the night before.
She assumes it’s just age. It isn’t.
A new study published this month in the American Journal of Epidemiology followed more than 7,600 adults over 50 for a full decade. What the researchers found was sobering. Adults experiencing significant financial decline lost memory function at a rate equivalent to an extra five months of biological aging every single year. Not people in poverty. Not people who’d lost everything. People whose financial footing was slipping — gradually, quietly, the way it does for millions of older Americans on fixed incomes when the world gets more expensive, and their income doesn’t.
Five months. Every year. That adds up fast.
The Body Doesn’t Know It’s Just Money
Here’s something worth understanding. Your brain has no category for “financial stress.” It only knows threats. When you lie awake doing the math on whether you can cover next month’s rent, your body responds identically to how it would respond if something were physically chasing you. Cortisol floods your system. Your heart rate stays elevated. Your nervous system locks into a vigilance state it was designed to hold for minutes, not months.
Prolonged financial strain overwhelms what researchers call “mental bandwidth”, the brain’s working capacity for everything that isn’t the immediate crisis. Memory, focus, emotional regulation, and decision-making. All of it competes with the constant background hum of financial fear, and all of it tends to lose.
This isn’t evading responsibility. It’s also not poor coping. It’s what chronic stress does to any human brain, regardless of how tough or resilient you are.
Sleep Is Where It Compounds
The cruelest part of this cycle is what happens at night. Financial anxiety is one of the most reliable destroyers of sleep quality there is. Economic stress produces insomnia and fragmented sleep, which deepen exhaustion and sharpen anxiety the following day. So the thing most capable of restoring your brain’s sleep is the thing financial stress most reliably steals.
And sleep isn’t just rest. During deep, slow-wave sleep, your brain does its most important maintenance work. It consolidates memories. It clears metabolic waste, including the proteins associated with Alzheimer’s disease. It recalibrates the stress hormones that, when left unchecked overnight, continue eroding the hippocampus — the brain’s memory center. Even a single night of poor sleep has been shown to increase beta-amyloid accumulation in the hippocampus, the kind of accumulation that, repeated over years, becomes something much harder to reverse.
This news is why the Columbia findings hit so hard. Financial decline doesn’t damage memory in some abstract, statistical way. It damages memory through a very specific, very physical mechanism — chronic stress disrupts sleep, disrupted sleep degrades hippocampal function, and degraded hippocampal function accelerates the exact cognitive changes that aging adults fear most.
The Number That Should Change Everything
The study found something else that matters deeply for anyone trying to help people in this situation. Improving someone’s finances did not consistently reverse the cognitive damage that had already occurred. Decline predicted decline. Recovery did not reliably predict recovery.
That asymmetry carries a message: the time to intervene is not after the situation improves. It’s now, with whatever tools exist for addressing the neurological effects of stress that financial circumstances can’t immediately fix.
You cannot hand someone a better pension. You cannot change the cost of groceries or the interest rate on their debt. What you can address is what all of that stress is doing to their brain while they sleep, or fail to.
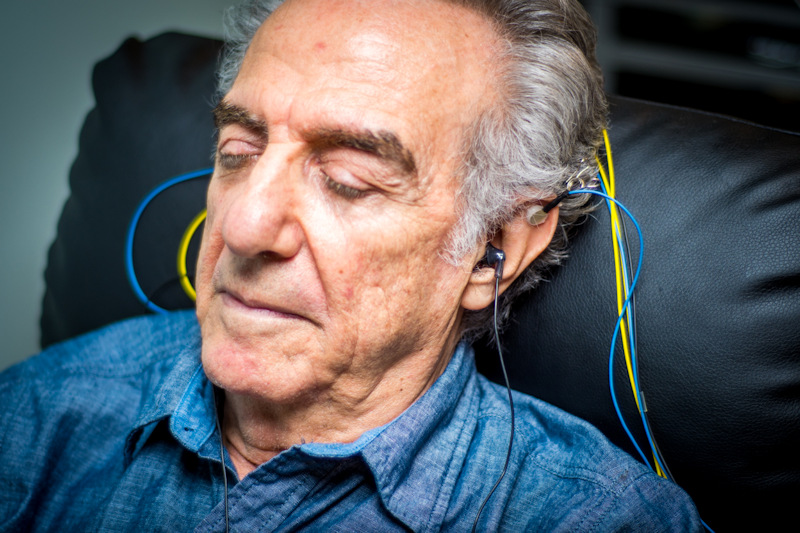
Something That Can Actually Help
A nervous system locked in chronic financial anxiety develops a recognizable pattern. On an EEG, it shows up as a brain that cannot downshift. High-frequency activity stays elevated when it should be tapering. The slow, deep oscillations the brain needs for restorative sleep are suppressed. The system is running a threat-detection program around the clock because, from its perspective, the threat never left.
Neurofeedback for seniors works by training the brain toward more efficient, flexible oscillatory patterns, specifically those that support deep sleep. Not by sedating it. Not by artificially suppressing the stress response. By gradually teaching the brain that it’s safe to slow down, that the restorative states it needs are accessible even when circumstances are hard.
What Clients Actually Experience
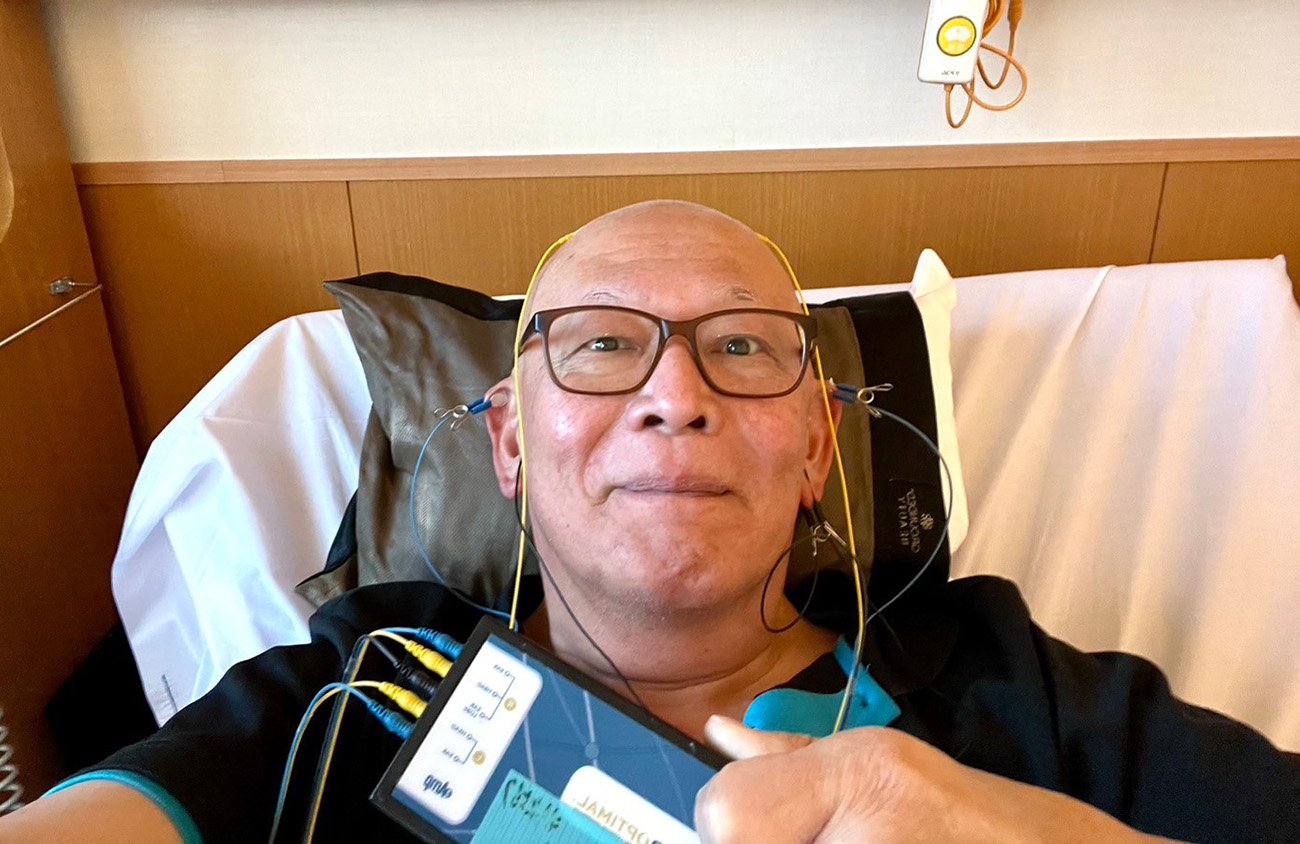
The changes tend to be subtle at first, which is exactly how real neurological change works. Most clients don’t wake up after their third session, announcing that everything is different. What they notice, usually somewhere between weeks two and four, is that they’re waking up slightly later. That the 3 a.m. ceiling-staring has gotten shorter. That they’re falling back asleep instead of lying there cataloguing everything wrong.
From there, the picture tends to fill in gradually. Anxiety that felt constant starts feeling occasional. The financial worries don’t disappear, the rent is still due, the pension is still what it is, but the brain’s relationship to those worries begins to shift. There’s more space between the thought and the spiral. Clients often describe it as feeling less reactive, less braced. One woman recently told us she’d stopped keeping the calculator on the nightstand. Not because her finances had improved, but because she’d stopped needing to run the numbers at midnight to feel in control.
Sleep architecture changes follow. Clients begin reporting deeper sleep, more vivid dreams, mornings where they wake up feeling like the night actually did something. Those are signs of restored slow-wave activity: the brain cycling properly through the stages it needs to consolidate memory, clear waste, and reset the stress response before morning.
Cognitive sharpness tends to return quietly, too. Clients mention remembering conversations better, finding words more easily, and feeling less foggy in the afternoons. These aren’t dramatic before-and-after stories. They’re the slow accumulation of nights that are finally doing their job.
For older adults living under sustained financial pressure, this trajectory matters enormously. The Columbia study makes clear that the cognitive cost of chronic financial stress is real, measurable, and accumulating. But a nervous system that has learned to downshift so it can move through the night without staying on guard stops paying that cost the way it used to. The finances may remain the same. The brain doesn’t have to.
